While writing “Not My Problem” Healthcare: Cultural and Societal Ethics, many questions about healthcare and the experiences of patients and caregivers who advocate arose. Like..
Why are derisive adjectives, (like “difficult” and “demanding”) used to label patients and caregivers who ask hard questions?
Why is shunning of vulnerable people occurring?
Where is compassion?
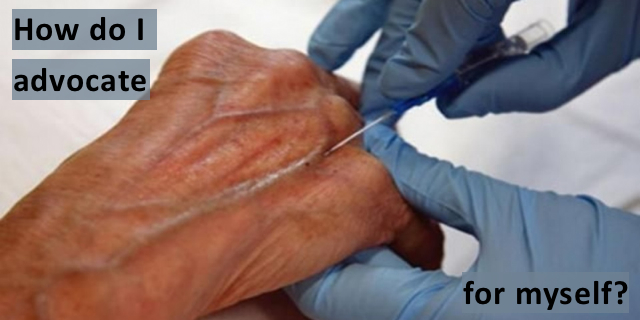
How Do I Advocate for Myself?
Patient advocacy is complicated by the power dynamic that exists in the provider-patient relationship. Faced with this reality, patients and caregivers want to know how to advocate for themselves and not suffer because they do. In fact, one reader sent a list of questions that we are going to try to answer in a series of posts.***
- How should both patients and doctors manage the diplomacy of patients being their own care coordinators?
- How can you get the attention of a specialist without drifting into seeming to be a know-it-all?
Providers Who Have Been Patients
Two people with extensive experience in the healthcare setting as both providers and patients can provide some answers. Stephanie Zimmerman, is a pediatric oncology nurse practitioner living in the US. Featured in After Cancer Treatment: Living Out the Cure, Stephanie is a childhood cancer survivor who at age 38 needed a heart transplant due to damage caused by the treatment used to cure her cancer. She is cohost of a weekly social media discussion #AllThingsCancer. Kathleen Thompson, MD is a physician specializing in pharmaceutical drug research in the UK. A breast cancer survivor, Kathleen is the author of From Both Ends of the Stethoscope: Getting through breast cancer – by a doctor who knows.
Kathleen Thompson’s Advice
Kathleen’s answer to the two questions begins with an acknowledgement of the power dynamic of the doctor-patient relationship.
“The doctor-patient relationship is intrinsically unequal. When we are ill, we are vulnerable, and we tend to avoid ‘upsetting’ or angering the person who holds power over our life and health….As a doctor, having breast cancer was an eye-opener – even I found it difficult to assert myself when I became a patient.”
Kathleen provides a list of ideas and resources* that can help. She recommends,
“1) Take someone with you
Two pairs of ears are better than one, and it is easier to challenge things with the moral support of someone close.
2) Increase your level of knowledge
Read as much about your illness as possible.
3) Understand your self worth
To get the best out of the healthcare system you must value yourself. Do not worry about upsetting your doctor. Remember that a conscientious doctor will be only too glad to be know that, either (1) you have not understood and need further clarity or (2) he was inadvertently suggesting an incorrect solution. If your doctor takes offense, frankly, your life and health is more important. [emphasis added]
A quick assertiveness course:
a) If you need something speak out
b) Your needs are as important as everyone else
c) Make yourself speak a little slower and louder than normal
d) If you are unclear about what you are being told, request further explanations until you are confident you have understood – do not leave until you are sure
e) Be polite but firm”
Her final word?
“Should we challenge our doctor? After all they are the experts, surely they know best? Well yes, usually they do, but we are the experts about ourselves.”
Stephanie Zimmerman’s Advice
An advocate is “one who pleads the cause of another”. [Noah Webster’s 1828 Dictionary]
 Stephanie has been an advocate for herself, professionally for children with cancer and their families and as a caregiver advocating for a loved one. “I have the benefit of the lived experience…Each of these roles has informed my approach to advocacy across time.”
Stephanie has been an advocate for herself, professionally for children with cancer and their families and as a caregiver advocating for a loved one. “I have the benefit of the lived experience…Each of these roles has informed my approach to advocacy across time.”
Her heart transplant at the Cleveland Clinic showed her what true collaboration among professionals can be. (please see Reduce Suffering In Healthcare for more on Cleveland Clinic’s initiatives)
“My team was huge…I watched them working and felt like something supernatural was taking place. I’d never seen people work together so well…Communication was seamless; everyone who saw me knew what the other specialists and team members were doing and what their goals were . Nobody on the team had an ego.”
But this is the exception rather than the rule. Advocating for oneself in the hospital is challenging, Stephanie notes, because of  “inadequate staffing despite the ever-increasing complexity of most clinical scenarios, the introduction of hospitalists, and an increase in the number of nursing assistants, coupled with a relative lack of adequate education taking on nursing practice with less than optimal supervision.”
“inadequate staffing despite the ever-increasing complexity of most clinical scenarios, the introduction of hospitalists, and an increase in the number of nursing assistants, coupled with a relative lack of adequate education taking on nursing practice with less than optimal supervision.”
These administrative, money-saving, trends impact the quality of care provided in hospitals. Because of this, Stephanie believes that you should never leave a loved one alone in the hospital. In addition she recommends these strategies for successful inpatient advocacy on the part of a family members, friends, and providers:
- “Kindness: treat the providers of care as you want your loved one or yourself to be treated and vice versa
- Honest Communications: if there are non-negotiables specific to your care, discuss that during your first encounter with your care providers; be proactive as it will preempt frustration
- Self control amidst [at times] great frustration: be firm in communications when necessary, yet again, be kind and self controlled with regard to your tone, volume, inflection, affect, and body language
- Gratitude: express it directly to the person in the moment; expressing interest in the care provider or the care receiver go a long way towards cultivating collaboration
- Apologies: be willing to accept responsibility for your words or actions even if that means a humble apology for poor behavior on your part
- Know your resources: you have the right to request a patient advocate at any time during the course of your inpatient stay
- Anticipate scenarios based on past experiences [chances are this isn’t your first rodeo]: develop and practice scripts.”
More to come
What are your thoughts and concerns about personal advocacy in the healthcare setting? What questions do you have? Please join this conversation in the comments section. There are more posts to come on this important topic.
Left bereft, we search for why, we quest for how, we wonder who. We don’t have answers, just more questions. Could I, would I, should I?
***In trying to answer these questions, the efforts that Jess Jacobs and her team of devoted friends and family is in no way being questioned. She and her team did everything they could to get her the compassionate, connected care she deserved. In fact, they utilized many of the suggestions in this post.
**Kathleen recommends Dr. Liza Macdonald’s website “Dealing With Your Doctor.” Click on the topics in the right hand column for specific ideas on working with your provider.






Recently my wife called 911 and I was transported to the hospital ER for a kidney stone (Number 15 for me). I’ve passed them all over time. I was eventually discard at 3 AM. The next day 1PM my wife called again, 911 due to excruciating right flank pain. I was told to remove all clothing and I was going to the OR. I was not given any explanation about the procedure by the staff or MD. “They will tell me in the OR and “Consent Me””??? I was reluctant. I explained I’m a healthcare provider NP and I got the same answer again. I told them I will not go until someone explains what was the procedure. The story also goes on after the Stenting of my right ureter. I have GERD and I take Dexilant daily. The only PPI that works and I hadn’t taken it for 3 days due to nausea and vomiting. I was told that they don’t stock it and it would be substituted for Protonix. I explained to the chief pharmacist that it doesn’t work and my wife even brought the medication to be used. I was told it was an “All or None” policy. I requested to speak with someone above her and was told there is no one above her. The moment I told her I was a health care provider the situation changed and I was granted my medication. Even though I had vomited a small amount of blood during the previous night. Had I not mentioned I was a healthcare provider who knows how this brief hospitalization would have turned out. Glad to be home. Now I understand why Hospitals many times have so many patient complaints in one for or another.
When doctors don’t have the answers why don’t they just say so, instead they just say come back in 6 months.
This advice is easier said then done. I’m a advocate and caregiver. I’m also a patient. It all depends where you are, what you have, your medical diagnosis and record, the reputation of your doctor, if your PCP is connected to the hospital and what time of day it is. I’ve had nightmare stories and beautiful experiences. And FYI, the Cleveland Clinic is in a class by itself and you can’t transfer your experience with them into any other place. They are exceptional and every healthcare facility should be like them. It is the only place that information works flawlessly.
Hi Janice, You have made some extremely valid points. Thank you so much for reading Medivizor. Kathleen
This is a very small issue, but any advice on what to say to get health-care professionals to believe me when I say I’m a hard stick? No one ever goes to get anyone else; they all feel that they will be capable. I feel like a prima donna if I say, “I need your best person at putting in an IV.” I understand that I can ask for someone else if they’ve stuck me 3 times without success. But I get tired of being stuck multiple times. Is that just life for a cancer patient? For example, yesterday, the RN couldn’t get a vein at my wrist and was going to put an IV into my wrist. I suggested instead a vein near my knuckle on my hand. A few days ago, a tech used a device to see my veins but still stuck me twice before he had to call someone else.
I’m a Veteran who also carries private insurance because of my need for good, compassionate, timely healthcare by providers I choose.
In the VA system, if you question, object, advocate for yourself, your labeled as disruptive, angry, upset, non-compliant, difficult and demanding. As an RN and a breast cancer survivor, reading my records after visits or phone calls makes me cringe. I’ve been portrayed as much of the above. Yet, I always maintained professionalism and courtesy at visits or via phone to the best of my abilities. Meaning- one can be beat down so much before you become frustrated. But the VA system wants their patients to be puppets, remain silent- do not under any circumstances question your care or advocate for ones self.
This is not what I was taught in nursing school and most definitely not what I expected of my own patients after school. I encouraged questions and challenges.
The VA Healthcare system is severely flawed. Veterans are unheard, berated, unjustly scrutinized, threatened and, if deemed unruly- wait listed.