You’re in the doctor’s office filling out paperwork. There are questions to answer about your health, but also about the health of your parents, grandparents and siblings. You scratch your head, panic a little, then leave lots of blank spaces, hoping the information won’t be relevant to today’s visit.
Regrettably those spaces–that missing information–may matter a lot.
According to the Surgeon General’s Family Health History Initiative, only a third of people in the US have tried to gather their family health history. Yet, in the case of cancer, your health history or heredity, can carry some weight.
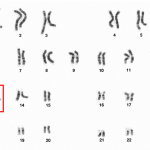 For example, the National Cancer Institute states that research has uncovered over 50 cancers resulting from a mutated gene inherited from a parent. These are called “hereditary cancer syndromes.” Only about 5% to 10% of all cancers are of this type.
For example, the National Cancer Institute states that research has uncovered over 50 cancers resulting from a mutated gene inherited from a parent. These are called “hereditary cancer syndromes.” Only about 5% to 10% of all cancers are of this type.
Sadly a 2011 study in the Journal of the National Cancer Institute reports that, overall people have difficulty being able to report cancer diagnoses in their family—they had “low to moderate accuracy” varying by the type of cancer. People were better able to report breast cancer, least able to report colon cancer. The issue was especially troublesome in reporting second degree family members: your grandparents, aunts, uncles, cousins and half-siblings.
Genetics, Family Health History and Genetic Testing
Knowing your family health history can inform you and your physician as to whether genetic testing is something you should consider.
Since Angelina Jolie’s public announcement of her BRCA diagnosis and preventative double  mastectomy, there have been many predictions of increasing use of genetic testing. In fact, an April 18 publication (via radio and online) of a story “More People Seek Genetic Testing, But There Aren’t Enough Counselors,” gives that impression. Yet polling data, from 2103 by Harris Interactive and from 2016 by Harvard STAT/Harvard T.H. Chan School of Public Health found that the number of people who have had genetic testing at only 8% and 6% of the US population, respectively.
mastectomy, there have been many predictions of increasing use of genetic testing. In fact, an April 18 publication (via radio and online) of a story “More People Seek Genetic Testing, But There Aren’t Enough Counselors,” gives that impression. Yet polling data, from 2103 by Harris Interactive and from 2016 by Harvard STAT/Harvard T.H. Chan School of Public Health found that the number of people who have had genetic testing at only 8% and 6% of the US population, respectively.
Genetic testing, especially for BRCA1 and BRCA2, costs less and is more available since the 2013 Supreme Court Decision stating that genes could not be patented (in 1996 Myriad Genetics had patented BRCA 1/2 mutations.) A plaintiff in this case, Ellen T. Matloff, Certified Genetic Counselor and President & CEO of My Gene Counsel, explains, “When BRCA1 and BRCA2 were first discovered, there were many labs across the country that were offering testing. Before the patent was overturned, the cost of BRCA testing was $4,000.”
Finding Certified Genetic Counselors
Certified genetic counselors are recommended by the American Cancer Society and the National Cancer Institute to help guide and explain genetic testing. Although the April 18 publication suggests a shortfall in numbers, people in hereditary cancer awareness advocacy disagree.
 Ellen Matloff is clear, “Patients should not get the message that they cannot see a certified genetic counselor if they need to do so. These professionals are available via phone, if you aren’t able to see a local counselor.”*
Ellen Matloff is clear, “Patients should not get the message that they cannot see a certified genetic counselor if they need to do so. These professionals are available via phone, if you aren’t able to see a local counselor.”*
In fact, “Certified genetic counselors are out there, available, and underutilized!” says Amy Byer Shainman, hereditary cancer advocate. “As a hereditary cancer advocate in the trenches (online support groups; talking to people on a daily basis about increased cancer risk) I hear it over and over again, ‘Where do I find a genetic counselor?’ ‘Can’t I just go to my regular doctor?’ One of the main things I do as a hereditary cancer advocate is tell people how to find a certified genetic counselor in their area. I tell them to go to the National Society of Genetic Counselor’s Find A Genetic Counselor Directory, enter city, zip and the specialty drop down is cancer –if a certified genetic counselor is not in their area, I tell them that Certified Genetic Counselors are available via telephone by going to http://informeddna.com .” **
The Importance of Family Health History: Lori’s Story
In a previous post on the Male Breast Cancer Coalition Medivizor shared Lori M. Berlin’s story.  Luck was on Lori M. Berlin’s side when her extended family communicated about their health issues. Lori, a former coordinating producer at ESPN, didn’t know her family in New Orleans until, out of the blue, her father’s cousin, Bernard, reconnected with the New York side of the family. Bernard had just been told he had metastatic cancer. Testing revealed the cancer originated in his breast: metastatic triple negative breast cancer (TNBC). Strangely enough, Bernard’s daughter had just fought TNBC, twice.
Luck was on Lori M. Berlin’s side when her extended family communicated about their health issues. Lori, a former coordinating producer at ESPN, didn’t know her family in New Orleans until, out of the blue, her father’s cousin, Bernard, reconnected with the New York side of the family. Bernard had just been told he had metastatic cancer. Testing revealed the cancer originated in his breast: metastatic triple negative breast cancer (TNBC). Strangely enough, Bernard’s daughter had just fought TNBC, twice.
Yet, “There really wasn’t any reason for me to think that I had the [BRCA] mutation. There wasn’t any breast cancer or ovarian cancer…with the women in my family,” Lori said in an interview.
“I had to fight and fight to get my testing covered. My previous LCIS diagnosis and my dad’s first cousin with male TNBC were not enough. What was so important here was the family history to the genetic counselor.” Lori stated.*** Because of her male cousin’s breast cancer diagnosis, genetic testing was approved.
Lori has the BRCA2 mutation. After disclosing the news to her family, both her parents were tested: she inherited the BRCA2 mutation from her father. Lori had preventative mastectomies and she believes, “Had I not known about a male with breast cancer (who was negative for BRCA), the genetic counselor wouldn’t have done the test. That’s why I say Bernard saved my life. Pathology showed I was going to get breast cancer in both breasts!” ***
Because her family shared their health history, Lori has been able to take precautions so that her risk of getting breast or ovarian cancer has been significantly reduced. Today Lori is an activist for the Male Breast Cancer Coalition.
Getting Started
 Knowledge is power. It may seem hard, but getting in touch with family members and sharing health information saves lives. There is an online tool at https://familyhistory.hhs.gov/ that can help you through the process. The website also provides a list family members to ask about health issues and questions to ask them. Take a look and let us know what you think.
Knowledge is power. It may seem hard, but getting in touch with family members and sharing health information saves lives. There is an online tool at https://familyhistory.hhs.gov/ that can help you through the process. The website also provides a list family members to ask about health issues and questions to ask them. Take a look and let us know what you think.
*Based on personal communication with Ellen T. Matloff, April 2016
**Based on personal communication with Amy Byer Shainman, April 2016
***Based on personal communication with Lori M. Berlin, November 2015

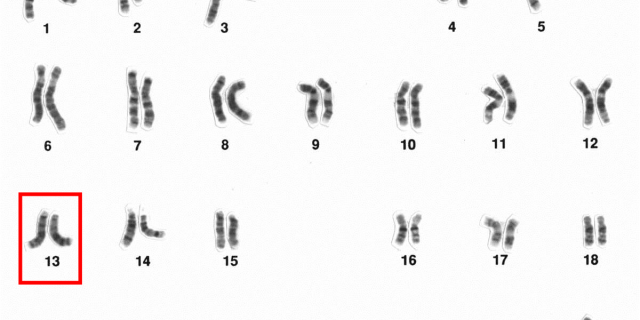





Lori’s case is a classic anticipated success story of how as the writer puts it, “knowledge is power” .. Leading to the preventative double mastectomy after knowing she has BRCA2 mutation. What more with the histopathology that probably showed up nuclear changes that led her to declare “Pathology showed that I was going to get cancer in both breasts.”
But let’s take a step back now and ponder.. Could a woman go through a similar preventative double mastectomy like Lori, after knowledge of having BRCA1 or BRCA2.. Yet discover later on from “Pathology” that tells her, “Oh, there are no cancer cells found.”
Would it be devastating to know, though she has a higher risk to get cancer by default of having the cancer genes.. to know realize “Hey, I may not actually get cancer at all !!??”
Hence, “Knowledge is Power” but so is Counsel. Good counselling from not just the medical professionals but also from friends, family and most importantly spouse. If you are a person of faith, then a prayer for wisdom is not inappropriate.. in order for the individual to collate all input and arrive at a final decision herself.. whether.. To Cut or Not To Cut..
Tq
Thank you for your insightful comment. Counseling from many sources, including genetic counselors, is vital in making such a life changing decision. -Kathleen