You may have heard of a treatment for the coronavirus (COVID-19) in the news that sounds unusual. It involves injecting serum from someone who has recovered from COVID-19 into patients who are sick with COVID-19.
Nobel Prize
This type of treatment actually won Emil von Behring the first Nobel Prize in Medicine in 1901.1 Behring was part of a cohort of medical scientists–including Louis Pasteur, Robert Koch, Paul Ehrlich–whose work in the late 1800’s and early 1900’s represents the dawn of immunological science.
Pasteur’s work on vaccines–made of attenuated but still live bacteria and viruses–to immunize people and animals from diseases like anthrax and rabies won him acclaim but also stimulated biomedical research in immunology. The Pasteur Institute, built in 1888, was a center of this research. And this center stimulated others in Europe to work in vaccines and immunity.
In Germany, Robert Koch identified the causes of anthrax, cholera and tuberculosis and used killed cholera bacteria to create vaccines that could confer immunity. Behring, working under Koch at the Institute for Infectious Diseases, began experiments injecting animals with attenuated diphtheria or tetanus. He took the blood from these animals, separated the liquid from the clotted blood cells (called serum) and injected the serum into animals who had already been infected with the full strength diphtheria or tetanus. The infected animals were cured by these injections.2
Although Behring’s serum was used in treating diphtheria in a child successfully, in 1891, Paul Ehrlich created a standardization protocol to enhance its effectiveness. The two men built a lab together and, using sheep and horses, began to produce larger quantities of the serum. In 1894 a joint venture with a chemical and pharmaceutical company produced anti-diphtheria serum in sufficient quantities to be marketed. For his work, in 1901, Behring won the first Nobel Prize in Medicine.
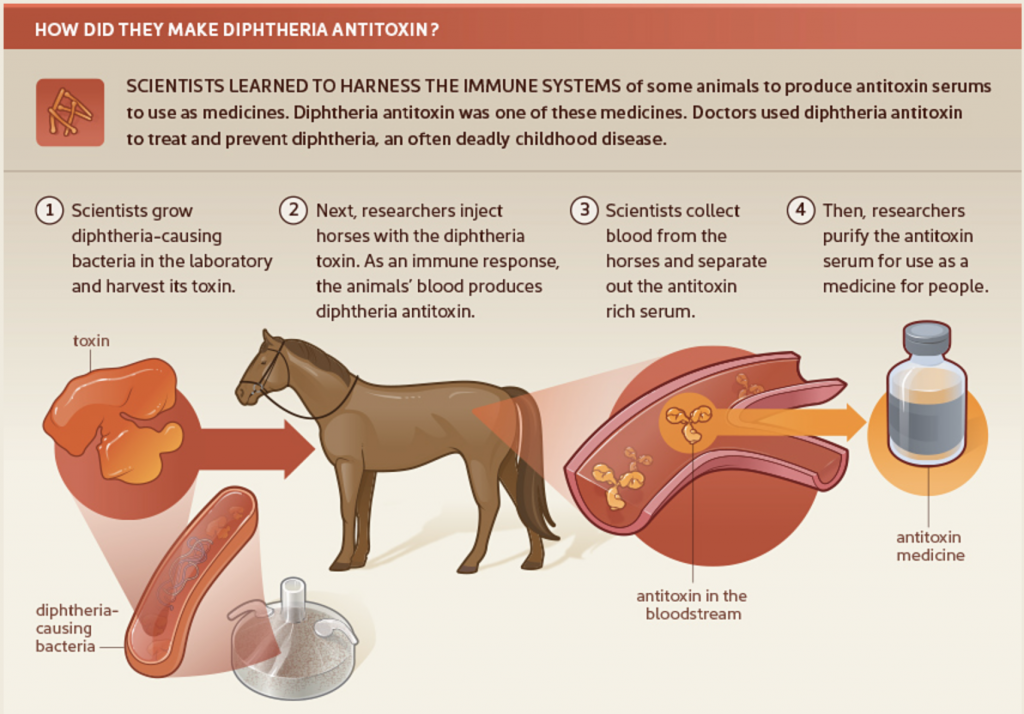
Serum therapy, now called passive antibody therapy, has been used both as a preventative of infection and as a post-infection treatment. Famously, convalescent serum therapy – obtaining serum filled with antibodies from people who have recovered from the disease – was used during the 1918 Spanish Influenza Pandemic. More recently serum therapy was used during the SARS and Ebola epidemics.2
How it works with viruses
When someone who is infected with a virus coughs or sneezes, viruses spread. If an uninfected individual breathes in the virus, the virus will colonize the epithelial cells of the respiratory system.
Many viruses have glycoproteins (a combination of sugar and protein molecules) enclosing their strand of RNA or DNA.3 These glycoproteins are seen as foreign by our immune system. Macrophages – cells in the blood stream and dispersed in tissues throughout the body – are part of the immune system. They ingest viruses and bacteria. They then display antigens to the glycoproteins of the virus on their cell membrane.
Macrophages travel through the lymphatic system to the lymph nodes and spleen and present these antigens to T-cells and B-cells. The T-cells bind with the displayed antigens and this binding activates the T-cells. They divide into 3 types of T-cells: Cytotoxic T-cells (which kill cells that are diseased or old), Regulatory suppressor T-cells (which moderate and control activity of T-cells) and Helper T-cells. Helper T-cells display the viral antigen receptors on their cell surface and are instrumental in the activation of B-cells.4
When helper T-cells bind with B-cells, the helper T-cells secrete lymphokines. Lymphokines activate B-cells to proliferate into two kinds of B-cells: Memory B-cells (cells that aid in future immune responses to this type of virus) and Plasma cells (which produce antibodies to the specific virus that is attacking the body).
Here is a video which animates this process.
The antibodies remain in the blood stream of a person (or animal) that has been infected with the virus.
Using Passive Antibody Therapy for the Coronavirus
As in days of old, immunologists from John Hopkins are proposing obtaining the plasma of patients who have recovered from the coronavirus or COVID-19. That plasma contains antibodies that would give other people’s immune systems a boost. They have suggested that, by using present day blood banking techniques, this therapy could be used for medical workers who are being frequently exposed to the virus as well as to uninfected family members who are caring for infected family members. Passive antibody therapy would also help those having difficulty mounting an immune response, for example, the elderly or people taking immunosuppressant drugs for autoimmune disease, cancers and post-transplantation among others.
What do you think?
Please provide your thoughts in the comments section below.
References
1 Emil von Behring – Biographical. NobelPrize.org. Nobel Media AB 2020. Sat. 28 Mar 2020.
2 Graham, B. S., & Ambrosino, D. M. (2015). History of passive antibody administration for prevention and treatment of infectious diseases. Current opinion in HIV and AIDS, 10(3), 129–134. https://doi.org/10.1097/COH.0000000000000154
3 Qinghong Zeng, Martijn A. Langereis, Arno L. W. van Vliet, Eric G. Huizinga, Raoul J. de Groot. (2008). Structure of coronavirus hemagglutinin-esterase offers insight into corona and influenza virus evolution Proceedings of the National Academy of Sciences, 105 (26) 9065-9069; DOI: 10.1073/pnas.0800502105
4Rosendahl Huber, S., van Beek, J., de Jonge, J., Luytjes, W., & van Baarle, D. (2014). T cell responses to viral infections – opportunities for Peptide vaccination. Frontiers in immunology, 5, 171. https://doi.org/10.3389/fimmu.2014.00171
5Casadevall, A. & Pirofski, L. (2020). The convalescent sera option for containing COVID-19
J Clin Invest. 2020. https://doi.org/10.1172/JCI138003.
*Feature image from: https://upload.wikimedia.org/wikipedia/commons/b/b8/Gehrke_behring.jpg
**How did they make diptheria antitoxin image from https://www.nlm.nih.gov/exhibition/fromdnatobeer/exhibition-interactive/illustrations/diphtheria-alternative.html