Did you know that before the year 2000, poor pain management was called a major medical problem and was synonymous with poor medical care in the US? On January 1, 2001, Congress declared 2001 to 2010 the Decade of Pain Control and Research. Assuring that effective pain management occurred in hospitals, in 2003, the Joint Commission on Accreditation of Healthcare Organizations (JCOH) added pain management criteria to the requirements they establish for hospital accreditation.
Pendulum swings
Now, we are having an “opioid crisis.” The pendulum has swung back: instead of under medicating for pain, the concern is over medicating for pain. Why this pendulum swing? The answer has to do with the nature of pain, the painkillers our bodies naturally produce and our efforts to manage pain.
Subjective measures
Pain is measured subjectively because we haven’t figured out how to measure it any other way. Improving pain assessment tools has been a huge challenge. The pain assessment tool that’s commonly used in hospitals asks you to rate your pain on a 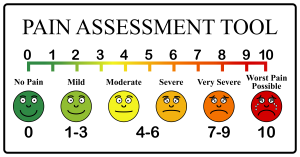 scale from 1 to 10.
scale from 1 to 10.
Pain is complicated. It is both physical and emotional. When we’re injured or experience some form of tissue damage, like when we burn a finger, we feel pain. All over our body there are nociceptors, sensory neurons (nerve cells) that respond to negative stimuli. The signals from these receptors travel to the spinal cord and then on to the brain. Interestingly, the places where pain messages are sorted out in the brain are the same places from which basic emotions, like anger and fear, are experienced.
Neurotransmitters
Pain research has focused on neurotransmitters: the chemicals involved in transmitting messages or signals from one neuron to another. The process involves passing signals through release of these chemicals in small packages (called vesicles) into the synapses (the space between the neurons). The 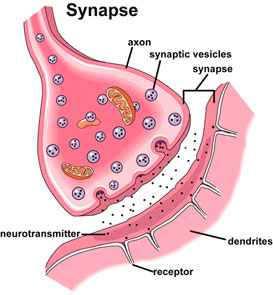 neuron receiving the message has a receptor protein on its surface that binds to the chemicals. The receptors have two responses, to open and move the message forward (excitatory receptors) or to block the message from moving forward (inhibitory receptors). TrpV1 is an excitatory receptor that is associated with feeling pain from heat. Another excitatory neurotransmitter is glutamate which has been implicated in persistent pain. Finding chemicals that will block glutamate will be instrumental in reducing pain.
neuron receiving the message has a receptor protein on its surface that binds to the chemicals. The receptors have two responses, to open and move the message forward (excitatory receptors) or to block the message from moving forward (inhibitory receptors). TrpV1 is an excitatory receptor that is associated with feeling pain from heat. Another excitatory neurotransmitter is glutamate which has been implicated in persistent pain. Finding chemicals that will block glutamate will be instrumental in reducing pain.
Opioids are neurotransmitters as well. Our bodies produce these pain killers naturally: an example of a natural opioid in our body is the endorphins associated with the runner’s high.
Morphine, either made synthetically or from poppies, is a pain medication that is like our bodies’ natural opioids. Because morphine can activate the opioid transmitters of the body, it is a powerful pain killer. But because it is so like what is produced by our bodies, it is also very addictive. *
Pain Is Different For Everyone
Everyone’s experience with pain is unique. Our different genetic make-up affects our pain sensitivity. Research has even identified genes involved in the process of feeling pain.
In 2011, the Institutes of Medicine estimated that over 100 million people in the US suffer from chronic pain. Sadly, the IOM also identified a cultural bias in the US against people who have chronic pain: specifically, those with chronic pain are seen as weak and thought to be lying about their pain.
In a forum where medical students ask practicing physicians questions on how to treat patients, the comments from physicians exemplify this cultural bias. These physicians were specifically speaking about patients who present to the Emergency Room with gastroparesis. One medical student wrote:
“How do you handle these patients? They come in saying intractable abdominal pain “I haven’t been able to eat or drink in a week!” and are generally on an absurd amount of pain medication. Then you get labs/imaging and there is nothing out of line. I hate these patients with a passion. My attendings always say “admit them for pain control and hydration” when there is nothing to fix. Now I am left trying to justify an admission to the hospitalist when every electrolyte is rock solid, their imaging is normal and they appear to be completely comfortable complaining of their pain. How do you guys deal with this in the real world? Or SHUDDER is it more of the same.”
One practicing physicianresponded,
“At my private hospital they ALL go home, I have never admitted for chronic pain.”
“I don’t see a lot of these in my current practice setting because my average patient is a 70-year-old retiree that fought several wars, lived through several recessions…overcame outstanding hardships, and understands that life is not without discomfort, pain, or difficulty.
It’s [gastroparesis] largely a disease of the young entitled wuss-crowd that has always thought that they could destroy themselves with cigarettes, alcohol, narcotics, high-fructose corn syrup, fast-food, and never have to deal with the consequences.
I like to tell them. Listen, I have (autoimmune disease). I am in daily 4/10 abdominal pain, yet you don’t see me in here bargaining for narcotics and applying for disability. I get over it.”
Still another believed that these patients want to “get put into a narcotic haze and have no responsibilities.”
 The response from people with gastroparesis can be found here. As Melissa Van Houton wrote, “It is absurd that we are put in a position where we have to FEAR going to an ER or a doctor because we might be mocked!”
The response from people with gastroparesis can be found here. As Melissa Van Houton wrote, “It is absurd that we are put in a position where we have to FEAR going to an ER or a doctor because we might be mocked!”
In her 2014 post published in Experts by Experience, Dawn Nellor, a patient with pulmonary sarcoidosis and chronic pain describes her experiences in this way, “The behavior of past appointments with physicians…have numbed me to their raised eyebrows and the “look-away” that represents disbelief.” She knows when “the arms crossed and the chair rolls back that the doctor’s next questions will be, ‘Are you sure it’s not stress?’ ‘Do you exercise?’ ‘Are you on antidepressants?’ ‘Why don’t you see your psychiatrist or try a different medication?’” As Judy Stone, writing about patients with rare disease in Forbes says, “A huge burden for patients with chronic pain and fatigue is being told that they are crazy.”
The post Not My Problem Healthcare is a description of someone with two rare diseases who wasn’t believed.
As Felice J. Freyer wrote in a 2016 story for the Boston Globe called, The Other Side of America’s War on Opioids, “As federal and state regulators rush to curtail access to drugs that have claimed thousands of lives, the rules they’ve enacted fall hard on people who legitimately need relief from pain [emphasis added]. In an atmosphere of heightened concern about opioids, patients in pain face reluctant doctors, wary pharmacists, and the frequent demand to prove that they are not addicts.”
Take Away
Since no one experiences pain in the same way, it might be time to take a deep breath and ask ourselves one question. Why do we blame victims of pain who need our help?
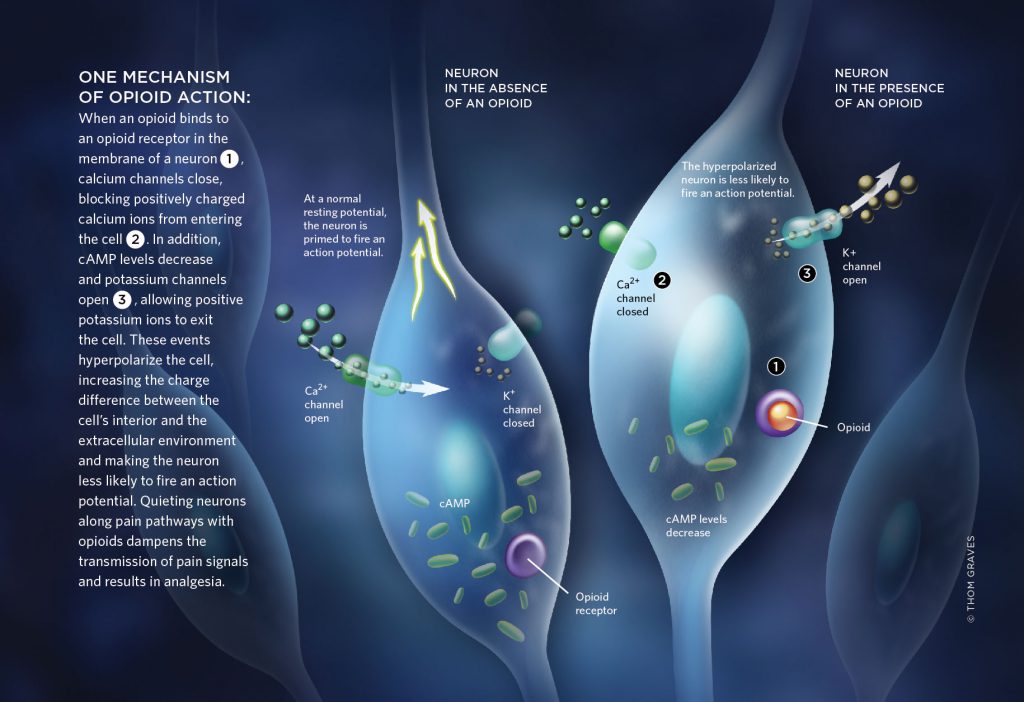
*Recent research has shown that glial cells, which are cells of the nervous system that support neurons, are involved in every experience of pain, including the experience of chronic pain. Glials cells have receptors called TLR4 that are activated when pain is experienced. Opioids also activate the TLR4 receptors. When the TLR4 is blocked, the analgesic action of drugs like morphine can be increased.







I am in constant pain from my cancer and as a result I have become addicted to narcotic pain meds and cannabis and botj seem to help. I have no problem with responsible Doctors prescribing narcotics for those in constant discomfort. I know that serious pain is real and that pain responds well to narcotics. Also people in serious pain will attempt to buy or just obtain narcotics of doubtful purity just to get relief. That is a terrible idea and often these people are forced into crime to obtain real pain relief. Just give them the drugs they need and get over the moral judgements about how terrible addiction must be , it isn’t!
Hello I totally agree with you I am terrified that my meds will be stopped!!
I couldn’t agree more. 1. Cancer patients should be exempt from any regulation. I took so much Motrin is desperation I screwed my stomach.
i have cronic pain in my back and left leg i was on pain killers i went off because i didn,t want to become hooked on them i have a fentaly patch it helps some but my pain is still at a 8 when i talk to my doctor about it he looks at me like i,m lying to him. how do i get him to under stand i,m really in pain i also have a lot of other illnesses
I live with chronic pain. Neuropathy and a recent fracture of the femur has produced such pain that I see a pain management physician and have to take daily pain medication. I could not continue to work and be somewhat productive without this help. Patients do suffer and if there is something that can help relieve this suffering and doctors are not assisting them then they should be ashamed of themselves. Sure, there are some who will abuse, but the majority of legit pain patients do not and should not be punished for those of us who are responsible. Shame on the medical associations for allowing this to continue to happen. Come up with tools for physicians to use to weed out the “drug addicts” who take pills for the high rather than the pain. There is a way. I know if the doctor who will not help a patient in pain were in pain themselves it would be a different story. Do not turn your backs on pain patients.
If I ever woke up with a pain level under 5, I’d think I was in Some one else’s body! When asked what my PAIN feels like, I try to give them an example from LIFE: toothache, ear ache, migraines, dislocation, fractures, and Kidney stones, child birth!
Gastroparesis is a very real, painful disease! I challenge anyone to spend one day in my shoes, or any other person suffering from this horrible disease! My body also has multiple autoimmune diseases such as Scleroderma, Fibromyalgia, and many others. My entire digestive tract is in complete failure and I survive on a feeding tube. I didn’t ask for any of this and definitely should not be shamed or questioned for requiring pain management.
Medical peeps: Nocebo is harmful. I work with people in chronic pain every day. Most will say that they need someone who will listen and believe their story. Empathy comes along side as a catalyst for relationship, trust, and a balanced approach to treatment. Your patients will get better if you stop blaming them for how they feel. Help the individual in front of you find what is the best treatment.
I have fibromyalgia & here in the UK it’s not seen as a disability, I am in constant pain & then a patient damaged my back & the pain shot up to a level that has left me completely incapacitated.
I got told to lose weight! I had already lost 2st (28lb) but the skinny Dr in front of me just saw a fat woman. He didn’t listen to anything I had to say. I’m a nurse who 3 yrs ago was working 45hrs a week – even with my fibro! I feel totally let down by my medical colleagues. They’ve been totally dismissive of me
I have been on opiates for years because my back is shot. Then I had cancer, fought it and won. Had major surgery in Oct. The wound had to be reopened in Nov and Ive had numerous complications. Then the Doctor dropped me and cut off all my meds. Cold turkey. Had pain off the charts and the ER Doctor at Spectrum Health Butterworth called me a junkie and refused to treat my pain. Ive been red flagged as an addict and cannot get another opiate pain medication in the state of michigan. Nice. Real nice.