E-health and mobile connectivity, coupled with powerful software, is hitting the diabetes community by storm. It’s a whole new world out there in self-care for people with diabetes.
Insulin Pumps
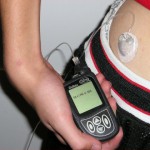 Rather than giving yourself individual injections of insulin every time you need it, an insulin pump provides you with rapid or short acting insulin continuously, on a 24 hour basis. Bolus insulin, for when you eat, can also be delivered by the pump, however you need to press a button for it to be delivered. You can also give correction bolus insulin if your glucose levels are high.
Rather than giving yourself individual injections of insulin every time you need it, an insulin pump provides you with rapid or short acting insulin continuously, on a 24 hour basis. Bolus insulin, for when you eat, can also be delivered by the pump, however you need to press a button for it to be delivered. You can also give correction bolus insulin if your glucose levels are high.
People like pumps because they don’t have to give themselves shots. It’s been found that pumps are more accurate in insulin delivery and often A1C levels improve with pump uses. People have also found that their lives are more flexible with regard to when and what they eat. They also tend to have fewer severe lows. The downsides include the feeling of being attached to a mechanical device all the time and the cost.
SMBG vs CGMs
There are a lot of acronyms in medical and diabetes care. Two are SMBG and CGM. SMBG stands for self-monitoring blood glucose and is the traditional way that people with insulin dependent diabetes keep up with their blood glucose levels. This involves frequently using a lance to stick fingers, test strips and meters to determine blood glucose levels.
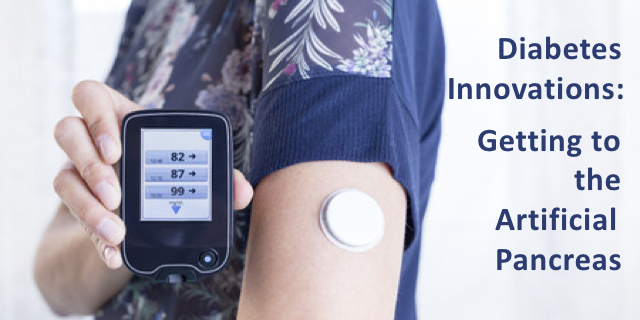
CGM stands for continuous glucose monitoring. These are wearable devices that track glucose 24-7. They include sensors which have to be replaced on a regular basis, adhesives to keep the sensors in place, transmitter and monitors/receivers. The sensors do 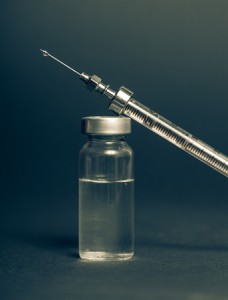 not test blood but test the fluid under the skin in the spaces in the tissue for glucose levels. These measurements occur every 30 seconds and are averaged every 5 minutes. The American Association of Clinical Endocrinologists as well as the Endocrinology Society have put out a joint statement saying that CGMs “may be appropriate for any person with diabetes who is willing to wear it, regardless of age, type of diabetes or duration of diagnosis.”
not test blood but test the fluid under the skin in the spaces in the tissue for glucose levels. These measurements occur every 30 seconds and are averaged every 5 minutes. The American Association of Clinical Endocrinologists as well as the Endocrinology Society have put out a joint statement saying that CGMs “may be appropriate for any person with diabetes who is willing to wear it, regardless of age, type of diabetes or duration of diagnosis.”
Cost is a large factor in the use of CGM. But, the ADA acknowledges the usefulness of continuous glucose monitoring systems for people with hypoglycemia unawareness. (see Diabetes 101: What is hypoglycemia unawareness?) Additionally CGM is considered useful for children, teens and young adults. Finally, if there is a suspicion of eating disorders, CGMs are a way to find out. (See 8 Signs of Eating Disorders in Insulin Dependent Diabetes)
The Artificial Pancreas
What is an artificial pancreas? At this point, it is not an implanted pancreas substitute. Perhaps it should really be called a closed loop system, joining the insulin pump with a continuous glucose monitoring device (CGM). The excitement around the closed loop system is that the software or algorithms involved “decide” on the need for insulin or glucagon.
These devices are in the works, with most product launches are expected in the US next year.
Why is an Artificial Pancreas so Important?
This question and its answer is for those who are not dealing day-in, day-out (or second-in, second-out) with the juggling it takes to  calculate insulin, keep up with carbs, exercise and deal with life. It takes enormous mental exertion to keep glucose levels within normal ranges. Unfortunately, even when someone is doing everything right, they may not stay within normal range.
calculate insulin, keep up with carbs, exercise and deal with life. It takes enormous mental exertion to keep glucose levels within normal ranges. Unfortunately, even when someone is doing everything right, they may not stay within normal range.
The ADA recommends self monitoring of blood glucose:
• Occasionally after meals (postprandially)
• When low blood glucose is suspected
• After treating low blood glucose until normoglycemia is achieved
With this amount of self monitoring and possible individualized injections, automation of some of the process can make an enormous difference for people with insulin dependent diabetes.
For more information
For detailed comparisons of devices, consider looking at Diatribe. Also, take a look at the American Endocrinologists Association website for patients.
And of course, check out Medivizor’s library: here’s a link for medical journal summaries on Insulin pumps, continuous glucose monitors and artificial pancreas.
Or get access to new, medical journal article summaries right to your email box by signing up for Medivizor.com.






Great – not! Been hearing 4 50 years cure 4 T1 was imminent. Technology is closer; Was on various pumps 4 over 25 years. Ho hum. The secret 2 tight control and better A1c s is CGM. Imagine my surprise when I found MEDICARE has tight restrictions on pumps 4 T1s AND DOES NOT COVER CGMS!!!That transcends idiocy and common sense. It’s cruel and inhuman btw.
Thank you for your comment. You have made excellent points! Kathleen